New Pathogens, COVID-19, and Antibiotic Resistance in the Field of Pneumonia










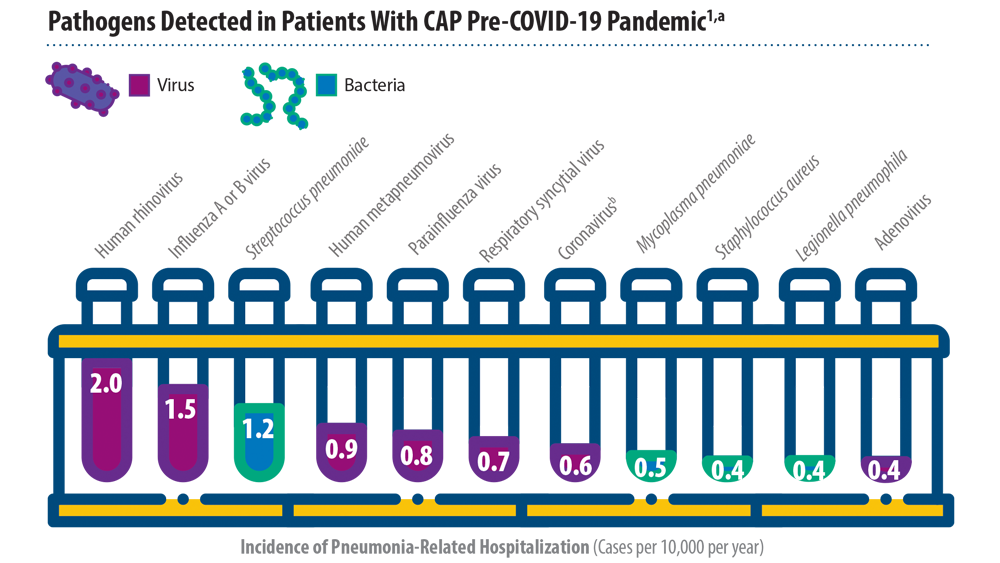
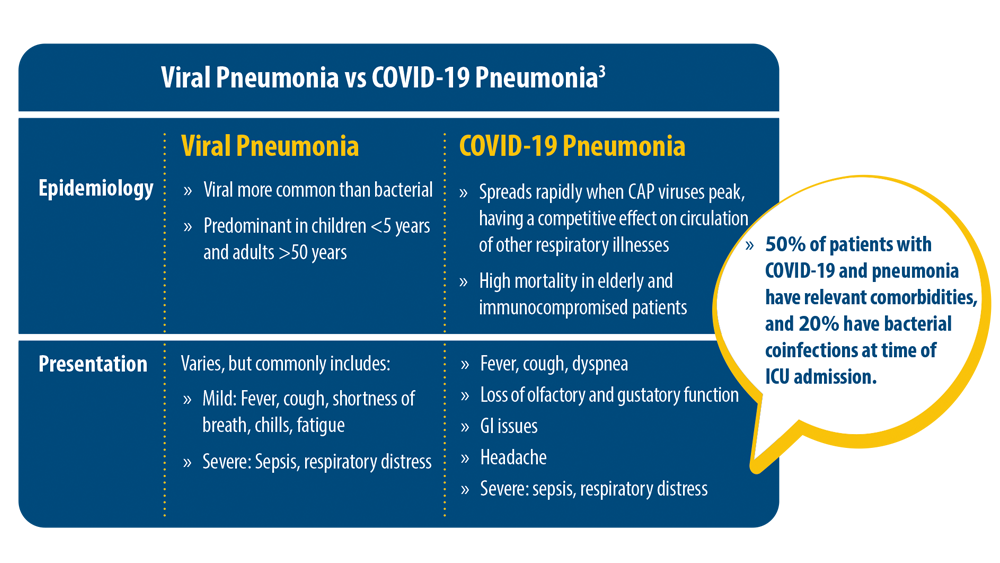
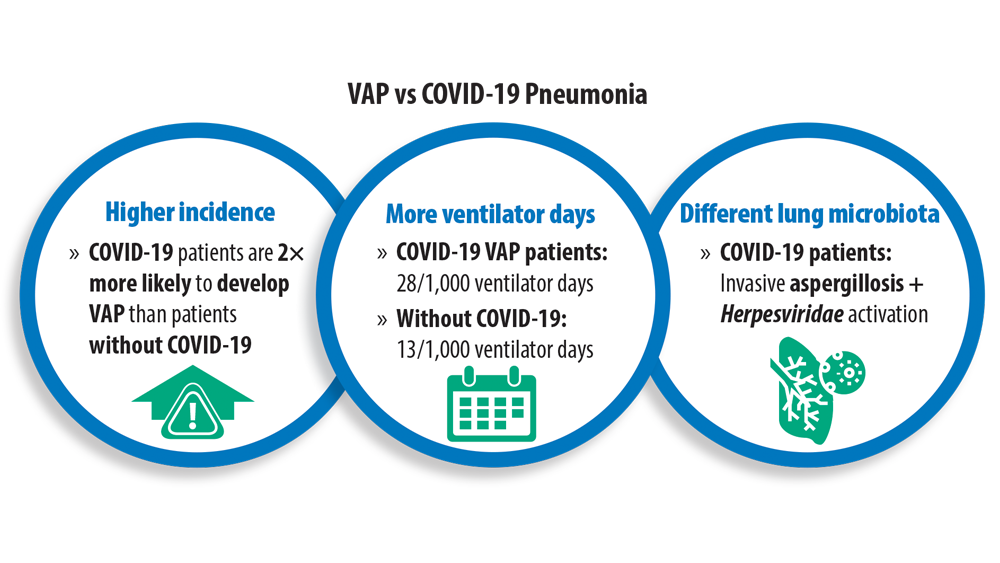
Before the onset of the COVID-19 pandemic, researchers in the feld of pneumonia were grappling with the increase in the number of pathogens, antimicrobial-resistant strains causing pneumonia, and high mortality in short-term and long-term cases in those with comorbidites and with severe pneumonia.1,2 In 2015, a landmark study identified that the most common pathogens causing community-acquired pneumonia (CAP) were viruses such as rhinovirus and influenza virus, and that the most common bacterial pathogen remained Streptococcus pneumoniae.1 Just as the rest of world was forced to shift their focus in 2020 because of the pandemic, those of us in the pulmonary space were challenged to understand the impact that COVID-19 would have on treating our patients, particularly those with pneumonia. SARS-CoV-2, the virus that causes COVID-19, in a short time became the leading pathogen causing pneumonia. In addition, severely ill patients with COVID-19 were found to have a higher risk of developing hospital-acquired pneumonia and ventilator-associated pneumonia (VAP). The rate of VAP increased during the pandemic due to several factors, one of them being the time patients with COVID-19 spent on ventilators.3,4
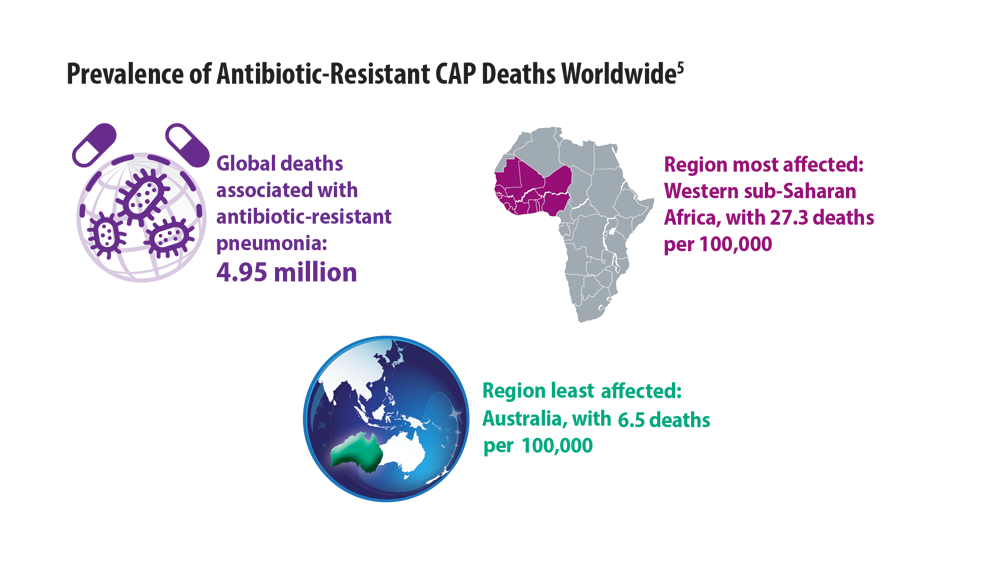
Now that the pandemic has passed its peak, the field of pneumonia is revisiting earlier concerns—assessment of new pathogens and antibiotic resistance—as well as addressing issues brought to light by the COVID-19 pandemic.